The Danish health system differs from the Czech one in that a major part of the responsibility for the prevention and provision of health care lies with the local government, as well as a long tradition of public-private partnerships. This enables us to offer innovative solutions that respond effectively not only to the needs of patients, but also to rising healthcare costs due to chronic diseases, Jakob Skaarup Nielsen believes. The CEO of Healthcare Denmark spoke about Denmark’s approach to prevention at the 2nd Annual International Panel of the Permanent Conference on Healthcare in Prague.
Effective prevention is absolutely essential to the financial sustainability of our healthcare system. Everyone needs to be encouraged to lead a healthy life, said Jakob Skaarup Nielsen at the 2nd Annual International Panel of the Permanent Conference on Healthcare. The CEO of Healthcare Denmark, a non-profit organization, is also convinced that the key to truly effective interventions are multidisciplinary public-private partnerships.
„We need support from the private sector. We continue to examine how to combine the knowledge and experience of industry with public health services. Our goal is to offer new innovative solutions precisely targeted to the needs of patients and citizens,“ says Nielsen. He adds: „We see a clear global trend in the industry where companies are moving from being suppliers of products to providers of services. They resort to this to remain competitive. And we in public health need to take advantage of that.“

Health on a mobile phone
Denmark is known for its long tradition of partnerships between the public and private sectors. It is also the basis for Healthcare Denmark, which is headed by Nielsen and half-owned by the state. Such cooperation, combined with the fact that responsibility for prevention measures in Denmark lies largely on the shoulders of local authorities, makes it possible to set up effective prevention measures and offer them directly to the people, according to Nielsen.
For example, on their mobile phones. As an example, Nielsen cites the Live App mobile app developed by Liva Healthcare. This was in response to the fact that approximately one third of Danes over the age of 16 suffers from at least one chronic disease. This app therefore offers digitally tailored support for healthy lifestyles and disease management. „Local municipalities have also collaborated in its development and are also using and offering it extensively,“ explains Jakob Nielsen.

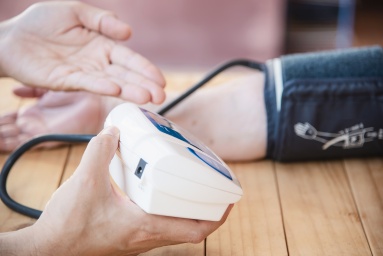
The app allows the monitoring of movement, sleep, the nutritional values of consumed food, as well as blood sugar, blood pressure, etc. It also offers personal lifestyle advice or communication with a doctor. „The app has provided significant health improvements to its users. For every diabetic with the app, local governments save $2,360 (roughly CZK 50,000 – ed.) annually compared to those who do not use it,“ Nielsen points out. Not to mention the fact that people living in less accessible areas have easier access to information about their health.
Risky behaviour is an expense in itself
In light of the fact that public spending due to chronic diseases is still rising and will probably not stop doing so, this is not an uninteresting figure. „It is important to recognize that the economic impact of risky public behaviour is huge. Risky behaviour is an expense in itself, as it is directly linked to the development of many chronic diseases,“ Nielsen points out.
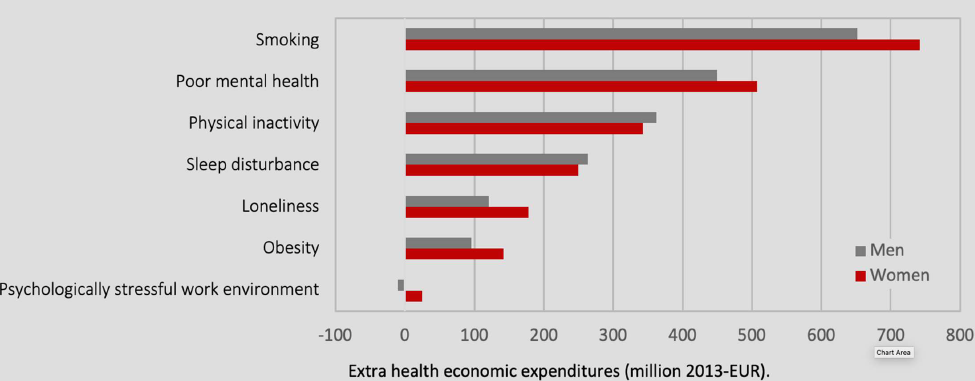
In Denmark alone, he says, the number of patients with type 2 diabetes will almost double by 2030 compared to 2015. „And that will put an even greater health burden on our system. Already today, health care costs related to chronic diseases account for 80 percent of the total budget. We need to address this today and in the future, otherwise we will stop being able to manage the situation,“ says the Director of Healthcare Denmark.
This is why Denmark pays considerable attention to primary prevention. However, the Danish Health Institute (Sundhedsstyrelsen) works closely with the local authorities, who, as already mentioned, are the ones with main responsibility in this area, providing them with information support and advice on the best way forward. So far, it has issued such support material in eleven areas: alcohol, tobacco, obesity, mental health, physical activity, hygiene, the indoor environment in schools, food and nutrition, sexual health, drugs, and sun protection.

Nielsen cites recommendations for obesity prevention as a concrete example. For example, in settings that care for preschool children, staffs are given instructions on how to promote healthy eating, physical exercise, and a general awareness of healthy lifestyles among children.
This is also an area where the benefits of public-private partnerships can be exploited, including at the international level, says Nielsen. An example is the current cross-disciplinary project of an international consortium, poetically called the Danish Lighthouse of Healthy Weight. It aims to find and develop new tools for the prevention, early detection, and management of obesity. And if they prove successful, such partnerships can be introduced to other areas such as geriatric care or psychiatry. The planned sub-projects also include the use of virtual reality or artificial intelligence elements. The first results of this partnership should be presented at the Healthy City Summit next autumn, adds the Healthcare Denmark director.
Helena Sedláčková